“Personal trainers and fitness professionals see clients with symptoms of OA all the time, but unfortunately the basic qualifications don’t provide enough information and guidance about what and what not to do with them. We need quality, academically-sound courses for personal trainers on injury and rehabilitation to effectively manage these conditions.”
Before we get stuck in, first, let’s briefly cover the basics.
What is Osteoarthritis?
Osteoarthritis (OA) is a type of joint disease that results from breakdown of joint cartilage and the underlying bone. The condition most commonly affects the joints in your body that carry weight, such as the knees, hips and spine. The main symptoms of this condition include pain and stiffness, which can get worse following weight-bearing activity. The last treatment option, particularly in the knees and hips is joint replacement. We’ve covered this in a previous news item, see here for more details.
Ideally, we don’t want to leap into major surgery, so what can be done to manage this condition and indeed is there anything that can be done to improve the symptoms? Well, let’s look at the problem in more detail.
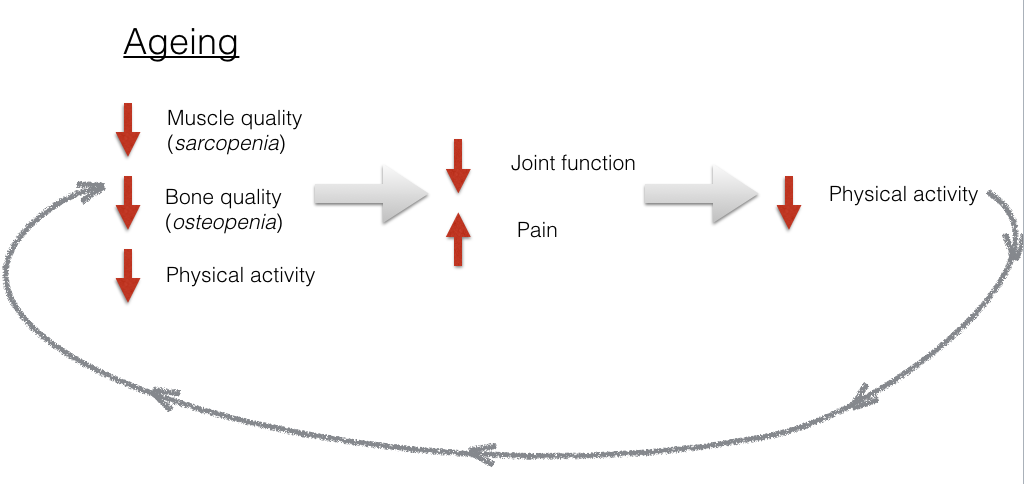
The problem mainly affects older people (>50 years). Look the diagram below. As we age, the quality (strength, flexibility, amount) of our tissues such as muscle and bone decreases. These processes:
- sarcopenia: loss of muscle mass and muscle quality and
- osteopenia: loss of bone mineral density
occur naturally. Unfortunately, as we age our tendency to take part in physical exercise also decreases.
So we have a naturally declining physical functional capacity, that is compounded by a lack of exercise. Why does a lack of exercise make things worse? Well the stress and load associated with doing exercise causes the tissues to adapt and become stronger. And, as we know, the muscles surrounding a joint are hugely important in maintaining its normal function and stability.
Spiral of decline
What can happen next, particularly with OA is that a decline in muscle function means that the function of the joint i.e. how well it can move, also declines. This then increases the symptoms of pain and stiffness.
If a person has a painful and stiff joint, you can forgive them for not putting exercise at the top of their ‘to do’ list! .. so they limit their physical activity further. And then we loop round and the process continues. I’m sure you can see, how by not engaging in exercise they symptoms of OA can become worse..?
What exercise to do?
Exercise is a recommended treatment for osteoarthritis. In fact, I would say that it’s a must, and you don’t have wait until you have OA!
Personal trainers and fitness professionals see clients with symptoms of OA all the time, but unfortunately the basic qualifications don’t provide enough information and guidance about what and what not to do with them. We need quality, academically-sound courses for personal trainers on injury and rehabilitation to effectively manage these conditions.
In simple terms, exercise comprising a mixture of aerobic and resistance training is advocated. The way in which to deliver this, however, becomes more complicated when your client has stiffness and pain, which may get worse with weight-bearing activities. You need to become creative with your exercise selection and exercise adaptation.
If we focus on the muscles for a moment, I would say don’t be afraid to go heavy on the weights. Naturally, ensure this is in a safe and controlled environment and you must be guided by your client’s symptoms, but the bottom line is training the muscles to stabilise the joint requires a different focus to your typical 12-15 RM.
How to resistance train for joint stability?
I’ve covered this in a previous article, which focussed on skiing. Obviously your client group is different here, however ,the principle is the same. We need to focus on the fast-twitch capacity of the muscle. Why? To develop the capacity for rapid force production.
Injuries resulting from stumbles, trips and falls often occur because the person was unable to right themselves in a timely enough manner – i.e. their muscle force production to correct their posture or perform an evasive manoeuvre wasn’t rapid or strong enough. Control, or proprioception is important, however, this needs to be trained separately.
So, what to do? First make sure your client warms-up. This is really important in an OA population. Second, what is the severity of their symptoms right now? What causes them pain, how much pain, are they in any discomfort presently etc. Once you have established this, and of course that they’re certified clear to exercise you can start to develop your programme.
There’s too much on this topic to cover in this article, however, let’s just take a really simple example:
Your client complains of discomfort doing knee extensions when they start with their knee flexed to 90 degrees or more. What do you you do..?
- Find a pain free range. Set up the machine to work the quadriceps towards the end of the range, for example start the exercise at 60 degrees and work up to full extension.
- Consider the mode of muscle activation. Powerful concentric muscle contractions elicit symptoms, however, what about isometric contractions? There’s a transfer effect of isometric training across joint angles (especially at long muscle lengths). Set the machine up so the lever arm doesn’t move and identify 3 joint angles where strong, powerful muscle contractions elicit fewer or no symptoms. Concentrate on ‘explosive’ fast activation (once warmed-up!)
Exercise adaptation
If you want to learn more about how to train people with injuries, how injury affects muscle performance and creative strategies for exercise adaptation
Click here for exclusive programme!