Hi there. Welcome to post 17 of the Strength and Conditioning for Therapists series; I hope you’re well. I’m now back from the European Congress of Sports Sciences in Prague (which is why there was no blog last week) and raring to go. It was a brilliant conference, as always: 4 days of multiple and parallel sessions running on: sports physiology; training load; sports injuries and orthopaedics; psychology; sleep; muscle damage (and more) …. from 8am-8pm. 2,500 delegates from around the World; lots of new connections and collaborations formed and catching up with old friends.
Anyways, this week, I’m going to tell you about what we presented and how you can leverage our findings to enhance your own clinical practice.
Injury Means Deconditioning
So, with a musculoskeletal (MSK) injury, there’s usually an associated period of reduced activity, or in some cases total inactivity. The effects of both the injury and the decline in activity typically means that the individual deconditions. For example, a runner suffering an ankle sprain, a team games player picking up a hamstring strain, a recreational golfer injuring their back … in all cases it’s likely, unless they receive elite level support and attention, that each person will disengage from their activity – because it causes pain, and most likely don’t replace it with anything else. I’m sure you see this on a daily or weekly basis in your practice.
You might think, and perhaps rightly so, that this isn’t such a big deal in young, otherwise fit and healthy people. The deconditioning might not be so dramatic and normalcy can be restored fairly quickly, especially if the injury isn’t severe. However, with increasing severity of injury and, or, if the person requires surgery, the extent of deconditioning can be dramatic.
Effects of Surgery on Muscle Strength
I’m going to use the ACL (anterior cruciate ligament) as an example here because it’s so well studied, however, the premise is valid for other orthopaedic conditions too.

An individual ruptures their ACL, they fail conservative treatment and elect to have a reconstruction. Forgetting just for now the decline in neuromuscular performance that may have happened prior to surgery, what are the acute effects of the surgical intervention and rehabilitation limitations post-operatively?
Quadriceps muscle strength of the reconstructed limb typically declines by about 30% in the 10-weeks post ACL-surgery. (1)
That’s quite a lot, right? Now consider the rehabilitation and conditioning required to restore not only this deficit, but to improve performance to (ideally) above their pre-operative baseline. It’s not surprising that the literature reports significant quadriceps strength asymmetry that persists even after individuals have been cleared to return to sport (2).
Minimising Post-Surgical Strength Losses
Okay, so in most cases following injury or surgery where significant losses in performance are experienced, it, not usually clinically advocated to start strength training the muscle/joint at the point of injury. So how, if we can’t touch the limb, do we minimise strength losses…?
The Cross-Education Effect! I’ve spoken about this in a previous post – where you can experience the benefits of strength training on the opposite non-exercised limb (yes, it’s true!), but today I can tell you exactly what happened when we tried it in an ACL population in our clinical trial: the EFCOR project: “The Efficacy of Rehabilitation Exercise on the Non-operative Limb Following Anterior Cruciate Ligament Reconstruction“
We recruited 44 patients who elected to undergo unilateral ACL reconstruction and randomly allocated them to either:
- CE: Cross-Education Training Group (3 sets of 3-5RM lower limb resistance training, 3 exercises, 2 x per week on the non-operative limb) OR
- CON: A Control of time-matched upper-limb flexibility training
Everyone followed the same standardise ACL rehab, plus one of the above for 8-weeks post surgery. We measured patients pre- 10-weeks post and 6-months post surgery on a number of outcomes.
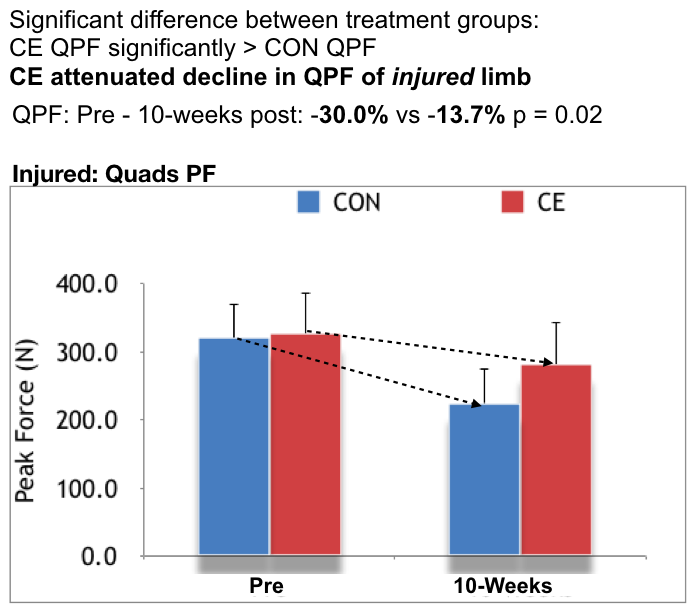
What did we find? Well, just like previous research, we saw a 30% decline in the strength of the quadriceps (QPF) in the injured limb of the CONTROL group when we tested at 10-weeks post surgery. … HOWEVER the CROSS-EDUCATION significantly attenuated this decline in the injured limb, they only experienced a 13.7% reduction in quadriceps strength (QPF) – see the figure below.
Summary: Does This Have Clinical Utility?
We still need to analyse all the neuromuscular data for the 6-month test, so I’m not sure yet whether or not these gains were retained once the cross-education training was removed. Furthermore, there were no significant differences at 10-weeks post or 6-months post-surgery in patient-reported outcomes (IKDC) or functional performance (hop). That said, this data adds to the evidence of a contralateral training effect, and if we view strength as an important rehabilitation and performance outcome in patient populations, which I think we should, then in my opinion this definitely has clinical utility.
Get In Touch
If you’d like to lean more about our study or the cross-education effect, drop me a line: info@getbacktosport.com or tweet me: @Claire_Minshull, I’d be happy to help.
COMING VERY SOON…..!
Please click below if you’d like to be notified directly about the DOWNLOAD that covers how to tailor your resistance training with patients to achieve specific goals and of the WEBINAR for a more in-depth look at this topic. Pop your name and email below and I’ll send you notification straight into your inbox. PLUS you’ll receive this weekly blog, and more to enhance your clinical practice
References
- Papandreou et al (2013). J Knee Surg. 26(1):51-8
- Kuenze et al. (2015). J Sport Rehabil. 24(1):36-46


