I hope you all enjoyed the couple of posts on EMD, what it is and how you can develop the specificity into your exercise programmes to train it..? Thank you for all the shares and RTs on Twitter and Facebook. The latter post in particular was pretty well-read with a few hundred hits 🙂
So we’re in week 11 and today I’m going look at assessment. I’ve been writing and producing a webinar for the great David Pope and his Clinical Edge platform over the past few weeks. Something that cropped up, but that I didn’t have enough time to cover in detail was the assessment of muscle strength in patient populations, and in fact this was one of the Twitter questions to me a few months ago. So thank you @ClemNihill, @RabbsPhiz and others for raising this. So let’s have a look at it today.
Measurement Characteristics
First of all, for an assessment of any index of function or performance to be meaningful, the test used:
- needs to be valid
- needs to have an acceptable level of reproducibility and reliability
- needs to be sensitive to change
Validity
The concept of validity was formulated by Kelly in 1927 and it basically means, is the test measuring what you’re think it’s measuring?… And accordingly how much meaning you can place on the results. For example, an IQ test should accurately measure IQ, and not memory, a test of strength should accurately test strength and not something else, like power, or endurance.
Reliability
Does a test yield consistent results on repeated tests. In the context of strength testing you want to know that a particular type of strength test will produce very similar results under the same measurement conditions, in the same person (if nothing has changed between tests). The measurement of any index of function – in humans – will vary a little between days and even within a session due to biological and technical error. People’s performance naturally varies a little over time (biological error) but the technical error – how precise or variable the test is should be controlled as much as possible.
A great example of the above is assessment of strength using isometric versus isokinetic testing. Creating a ‘solid’ isometric test whereby you minimise variability of equipment positioning, the person, and loss of information due to extraneous movement is easier than under isokinetic tests, or further, dynamic strength testing by lifting weights whereby movement is an essential part of the assessment. Creating the exact same movement pattern each time is exceptionally difficult. Therefore, the variability of performance scores during well-controlled and instrumented isometric testing is often much less than compared to isokinetic testing. In academic journals reliability, or reproducibility is measured by statistics such as Standard Error of the Measurement (SEM), coefficient of variation (V%), intra-class correlations (ICC) and Limits of Agreement (LOA).
On a single assessment of muscle strength in our lab on our custom-build dynamometer (see image below), the precision of measurement for strength is around +/- 4% (meaning that the score observed is within plus or minus 4% of the ‘real’ score), which becomes more precise (+/-2%) if we take an average of 2 or 3 measures (ref). Compare this to isokinetic testing, whereby precision might be +/- 10% (ref) and you’ll need to take the average of say 5 to 10 measures to achieve the same level of precision.
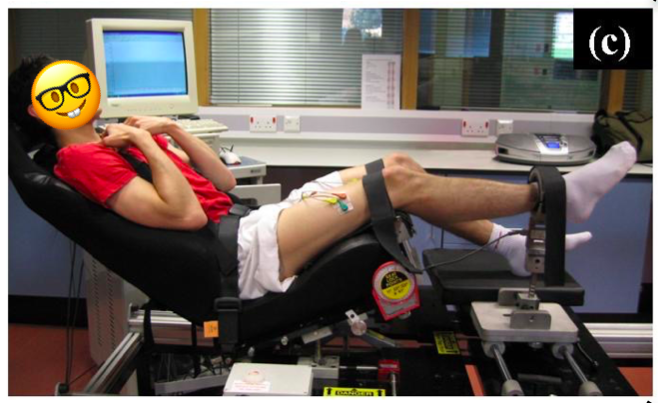
So, we should all opt for isometric testing…? Well, apart from resources, or lack thereof, the advantage of isokinetic and, or, more functional tests are that they are more dynamic and some view potentially more relevant to sport/daily activities
Sensitivity
Is the test that you’re using sensitive to change? Here you’re weighing-up how much change in strength is clinically meaningful and whether or not your chosen test can detect this, for example is a 1RM leg press assessment sensitive enough to detect a 20 Kg difference pre- to post-conditioning in healthy males? Probably. Is it sensitive enough to detect a 2Kg difference in rehabilitating patients, probably not. Again, a search of Google Scholar and PubMed will produce several results on what constitutes a minimal, or clinically-meaningful difference for the particular population that you’re dealing with. For example, Vaidya et al (2018), recently reported that a difference between tests of 7.5 Nm (roughly 73 Kg) constituted a meaningful difference in quadriceps strength measured by hand-held dynamometry in COPD patients.
Types of Strength Tests
As discussed above, we’ve got instrumented dynamometer tests, which include big and expensive isokinetic machines through to smaller and cheaper hand-held dynamometers. Incidentally, there are multiple research papers that document the reliability of hand-held dynamometry (HHD) in the assessment of muscle strength if you search PubMed or Google Scholar (here’s a link to just one [measurement error of 7.8-13%]). If you do have a HHD in your clinic, some of the most basic and important considerations to maximise the reliability and minimise the variability of a hand-held dynamometer test are standardisation and minimisation of extraneous movement so for example:
- attach the dynamometer to an immovable object, such as the leg of a bench for lower limb testing
- ensure the patient is stabilised and at least the tested limb strapped to the seat/bench
- standardise the anatomical placement of the dynamometer on the limb
- conduct several tests as a familiarisation
- give enough rest between efforts
- take an average of 2 to 3 efforts to generate the strength score
Not every clinic has access to dynamometry, so then we need to be little more creative and pragmatic in our assessments of muscle strength, whilst also bearing in mind the important measurement characteristics. Here we can opt for assessments of absolute weight lifted, for example a 1RM.
Verdijk et al (2009) that sought to determine whether 1RM testing is a valid means to assess muscle strength of the knee extensors, in a heterogeneous population by comparing it to other standardised strength assessments. Significant correlations between 1RM and isometric/ isokinetic peak torques were reported, which were stronger for leg extension than for leg press (most likely due to leg extension isolating the quadriceps more than leg press). The strongest correlation was found between 1RM leg extension and isometric peak torque (r = 0.88; SEE = 0.06, 95% CI = 0.81–0.93). So whilst there’s excellent agreement between muscle strength as assessed by 1RM leg extension and knee extension isometric peak torque, we’re not sure in this study of the variability of 1RM testing as the raw data wasn’t reported. Bottom line, 1RM probably isn’t as good as isometric assessments, but it’ll still give you some decent data to assess change.
Clearly, in patient populations, a 1RM isn’t always obtainable, so what can we do then to assess strength? Try to obtain a 3RM. This is still within the rep range for strength training and thus will give you some information on change and it might just be more tolerable than a single maximal effort. It’s likely that it’ll be less sensitive and more variable as a test, but certainly more objective than nothing.
And if that isn’t possible…? I guess a loaded functional test. How much weight is required to elicit a 3 RM sit-to-stand using a (very weighted!) backpack? Perhaps the same in a press-up position for upper limb testing…? In the absence of instrumented equipment, we’re reliant on creative thought and likely have to accept that most tests will be fairly imprecise and, or, sensitive.
Summary
This is a fairly broad overview of some of the different strength tests that can be used with patients. Next week I’ll focus more on the specifics and protocols of one or two. In the meantime, if you’re going to take a measure of strength make sure the test is standardised and repeatable, such that if you repeat the test again with the same individual any significant change in the score will be due to actual biological change and not due to variability of the test.
IT’S HERE! Download your Free 14-page guide: Strength & Conditioning for Therapists.

