SCROLL DOWN FOR FREE END-STAGE ACL REHAB … TO GET YOU BACK TO SPORT!
In the previous post we talked about the function of the ACL (anterior cruciate ligament), the mechanisms of injury and the lasting symptoms if you’re unlucky enough to injure it. Here we’re going to look at the ‘what next’…
Treatment of ACL Injury
What happens after you’ve injured your ACL will depend on the extent of injury an your sporting and activity goals. For example, if the ACL is only partially torn and your activity goals don’t include participating in activities involving lost of twisting, turning and changing direction, then conservative treatment may be an option. This involves a significant amount of muscle conditioning, especially of the hamstrings at the back of the thigh, which are the major protector of the ACL.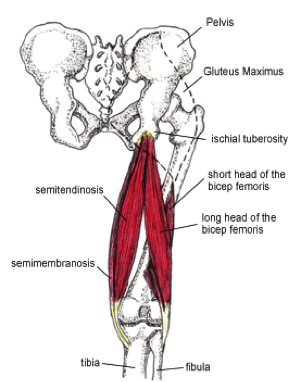
The hamstrings are the major dynamic protector of the ACL
This must include muscle strengthening, but also and importantly muscle conditioning to promote speed of muscle reaction and rapid force force production (Technically called: Electromechanical Delay and Rate of Force Development, respectively).
Rupture of the ACL takes less time than it takes to blink an eye!
If the knee is unstable and, or, you have aspirations to play sports then surgical reconstruction is usually required
ACL Reconstruction
The ACL is usually reconstructed using a person’s own tissue from the injured leg. Synthetic grafts are available, however, the lifespan of a synthetic graft is much less than a person’s own tissue and as such this type graft is used on rare occasions. The two most common grafts used are:
- bone-patella tendon-bone
- hamstrings tendons
Which graft you have will depend on things such as surgeon preference, the quality of your tissue, you occupation (if you’re a plumber you don’t want an extra problem of not being able to kneel properly for a few months, which is he case with a bone-patella tendon-bone graft) etc. Currently there’s no consensus on which graft is the best; research is just starting to be published comparing the long-term results of each. After surgery, the rehabilitation is much the same…
ACL Rehabilitation
 Arguably this is the most important part of the whole process. Why? Well, if you don’t get the rehabilitation right, you won’t experience the full benefits of the surgery. Rehabilitation should be a systematic scheduled approach to tissue loading, muscle conditioning and fine-tuning of your neuromuscular system to operate to protect you from future injury. For example, the rehabilitation needs to take account of the graft remodelling process in the early to mid- stages. Previously the graft acted as a tendon, now it must function as a ligament; it develops a new new blood supply and must strengthen to accommodate the forces placed through it. For this reason, heavy open-kinetic chain quadriceps exercises (knee extensions with weights & running) are typically avoided for the first 2-3 months following surgery.
Arguably this is the most important part of the whole process. Why? Well, if you don’t get the rehabilitation right, you won’t experience the full benefits of the surgery. Rehabilitation should be a systematic scheduled approach to tissue loading, muscle conditioning and fine-tuning of your neuromuscular system to operate to protect you from future injury. For example, the rehabilitation needs to take account of the graft remodelling process in the early to mid- stages. Previously the graft acted as a tendon, now it must function as a ligament; it develops a new new blood supply and must strengthen to accommodate the forces placed through it. For this reason, heavy open-kinetic chain quadriceps exercises (knee extensions with weights & running) are typically avoided for the first 2-3 months following surgery.
How Long Should ACL Rehabilitation Take?
Under optimal conditions, i.e. there’s no other pathology in the knee, you have regular access to the best physiotherapy, and you have the time to devote to your rehab, you could be back playing sport by 6-months.
Return to sport is possible 6-months following ACL reconstruction
You might find lots of information and articles talking about the quadriceps muscles, but beware… the hamstrings muscle are the major protector of the ACL. Thus any decent rehabilitation programme will have a specific focus on this muscle group, as well as the other knee and hip muscles.
The important bits that I find are left out of an ACL rehabilitation programme is the fine tuning end-stage rehab, which enables people to get back to sport. People often report that they’ve been discharged from physiotherapy, but the “knee doesn’t feel right” to get back to sport. For an active person, this is so important to restore sports-specific function and to help protect against re-injury. The important components of end-stage rehabilitation should seek to progressively develop quick muscle response times (electromechanical delay), fast rates of muscle force development and neuromuscular control (proprioceptive acuity)…in the appropriate sports-specific environments.
If you’re struggling with your end-stage rehabilitation, or if you’re a fitness professional who has a client as this stage and you’d like to know what to do. enter your details below and we’ll send you Stage 2 of an end-stage ACL rehabilitation programme for free!
[contact-form to=’minshullc@hotmail.com’ subject=’ACL rehab download request’][contact-field label=’Name’ type=’name’ required=’1’/][contact-field label=’Email’ type=’email’ required=’1’/][contact-field label=’Profession’ type=’url’/][contact-field label=’Comment’ type=’textarea’/][/contact-form]